血清胎球蛋白A水平與胰島素抵抗及頸動脈內膜中層厚度在初診2型糖尿病患者中的相關性分析*
黨玉婷,尹亮,孫侃,常向云
(石河子大學醫學院第一附屬醫院內分泌代謝科,新疆 石河子 832002)
血清胎球蛋白A水平與胰島素抵抗及頸動脈內膜中層厚度在初診2型糖尿病患者中的相關性分析*
黨玉婷,尹亮,孫侃,常向云
(石河子大學醫學院第一附屬醫院內分泌代謝科,新疆 石河子 832002)
目的旨在探討初診2型糖尿病(nT2DM)患者血清胎球蛋白A(FA)水平與胰島素抵抗(IR)及頸動脈內膜中層厚度(CIMT)的相關性。方法選取nT2DM患者100例作為病例組(T2DM組),糖耐量正常(NGT)者100例作為對照組(NGT組),采用酶聯免疫吸附實驗(ELISA法)試劑盒檢測血清FA濃度,計算穩態模型胰島素抵抗指數(HOMA-IR)評估IR,運用彩色超聲診斷儀測定CIMT,分析血清FA濃度與各項臨床資料之間的相關性。結果T2DM組血清FA水平(368.5±15.6)mg/ml高于NGT組血清FA水平(152.7±7.1)mg/ml,差異有統計學意義(=0.000);FA水平與HOMA-IR(=0.483,=0.000)、CIMT(=0.509,=0.000)、糖化血紅蛋白(HbA1c)(=0.153,=0.042)、三酰甘油(TG)(=0.353,=0.000)、低密度脂蛋白(LDL-C)(=0.113,=0.023)、體重指數(BMI)(=0.162,=0.024)、收縮期血壓(SBP)(=0.182,=0.035)、空腹血糖(FPG)(=0.422,=0.002)及2 h葡萄糖負荷血糖(2 h OGTT)(=0.581,=0.000)呈正相關,與空腹血漿胰島素(FINS)(=-0.153,=0.008)、2 h葡萄糖負荷血漿胰島素(PINS)(=-0.423,=0.008)、高密度脂蛋白(HDL-C)(=-0.183,=0.011)和HOMA-β細胞胰島素分泌指數(HOMA-IS)(=-0.463,=0.000)呈負相關。結論nT2DM患者血清FA水平與IR及CIMT之間存在相關性,研究結果表明,血清FA水平可作為診斷nT2DM患者大血管病變的獨立生物學標志物。
初診2型糖尿病;胎球蛋白A;胰島素抵抗;頸動脈內膜中層厚度
動脈粥樣硬化(Atherosclerosis,AS)是2型糖尿病(type 2 diabetes mellitus,T2DM)大血管并發癥的主要病理特征,也是T2DM患者死亡的首要原因。T2DM患者心血管疾病的發生率遠較血糖正常(normal glucose tolerance,NGT)者高[1]。部分初診2型糖尿病(newly-diagnosed type 2 diabetes mellitus,nT2DM)患者不具有典型的臨床表現,甚至幾乎不具有臨床癥狀,而高血糖是其唯一指征。因此,早期篩查高危人群可以采取有效的預防措施來降低T2DM患者心血管疾病的發生率和死亡率。
AS主要侵犯體循環中的心、腦、腎、外周動脈等大血管,其特征為斑塊形成,早期病變是動脈管壁內膜中層厚度增加。近年來有研究表明,頸動脈內膜中層厚度(carotid intima-media thickness,CIMT)能夠反映糖尿病(diabetes mellitus,DM)患者冠狀動脈粥樣硬化的程度[2],因此,早期發現DM患者頸動脈病變,盡早進行干預,給予及時的治療對于預防DM血管并發癥有重要的意義。
胰島素抵抗(insulin resistance,IR)是T2DM的主要病理生理機制,它可能促進T2DM和相關并發癥的發生和發展。IR也被認為是T2DM患者發生血脂異常和高血壓病的主要影響因素[3]。胎球蛋白A(Fetuin-A,FA)是由肝臟分泌的一種糖蛋白,是DM風險的生物標志物[4-9]。循環中高水平的FA可能與IR有關[10]。FA通過抑制胰島素受體酪氨酸磷酸化,導致細胞膜之間的胰島素受體的信號傳導發生障礙,引起胰島素抵抗[11]。另外,敲除小鼠胎球蛋白基因后觀察發現小鼠的胰島素敏感性增強[12]。此外還有研究發現FA能夠抑制異位鈣沉積、防止血管鈣化[13]。然而,關于FA在T2DM大血管病變中作為生物標志物的作用卻存在爭議[14-15]。
目前,nT2DM患者血清FA水平與IR及CIMT的關系未見報道。因此,本研究旨在通過檢測nT2DM患者血清FA水平分析nT2DM患者血清FA水平與IR及CIMT的相關性。
1 資料與方法
1.1 研究對象
選取石河子大學醫學院第一附屬醫院內分泌代謝科住院的nT2DM患者100例作為病例組(T2DM組)。其中男54例,女46例;年齡(55.11±12.84)歲;T2DM診斷標準符合1999年WHO制定的DM診斷標準。另取同期NGT者100例作為對照組(NGT組)。其中男44例,女56例;年齡(52.39±13.79)歲。T2DM與NGT組年齡、年齡段分布、性別及體重指數(body mass index,BMI)比較,差異均無統計學意義(>0.05)。排除標準:肝腎功能不全者,嚴重心腦血管疾病患者,頑固性高血壓患者,T1DM及特殊類型DM患者。本研究經本院倫理委員會批準,并按照赫爾辛基宣言的倫理指導方針進行。研究對象均簽署知情同意書。
1.2 血液樣本
所有受試者均于清晨9∶30~10∶00空腹(禁食8 h以上)采肘靜脈血3 ml,室溫靜置30 min,置于離心機中1 500 r/min離心10 min,分離血清,于-80℃冰箱保存用于檢測血清中胰島素及FA水平。
1.3 臨床資料
記錄受試者年齡和性別,測量身高、體重、腰圍、臀圍、收縮壓(systolic blood pressure,SBP)和舒張壓(diastolic blood pressure,DBP),計算腰臀比(waist-tohip ratio,WHR)、BMI、穩態模型胰島素抵抗指數(HOMA-insulin resistance index,HOMA-IR)及穩態模型β細胞胰島素分泌指數(HOMA-β-cell insulin secretion index,HOMA-IS)。采用葡萄糖氧化酶法測定空腹血糖(fasting plasma glucose,FPG)、2 h葡萄糖負荷血糖(2 h post-glucose load blood glucose,2 h OGTT)。采用固相放射免疫法測定空腹胰島素(fasting plasma insulin,FINS)、2 h葡萄糖負荷血漿胰島素(2 h plasma insulin after glucose overload,PINS)。由DS5糖化血紅蛋白檢測儀測定(配套試劑)糖化血紅蛋白(glycated hemo-globin,HbA1c)水平。采用酶聯免疫吸附法(enzyme-linked immunosorbent assay,ELISA)測定血清超敏C反應蛋白(high-sensitivity C-reactive protein,Hs-CRP)水平。采用全自動生化分析儀測定總膽固醇(total cholesterol,TC)、三酰甘油(triglyceride,TG)、高密度脂蛋白膽固醇(high-density lipoprotein cholesterol,HDL-C)、低密度脂蛋白膽固醇(low-density lipoprotein cholesterol,LDL-C)水平。
1.4 血清FA水平測定
血清FA水平測定采用ELISA法測定,試劑盒購于美國Epitope Diagnostics公司,實驗操作嚴格按說明書步驟進行。
1.5 CIMT測定
運用荷蘭飛利浦公司生產的IE33彩色超聲診斷儀(探頭頻率3.0~11.0 MHz)測定,病人取仰臥位,縱向超聲顯像可見相對低回聲分隔的兩條平行亮線,兩線間距離即CIMT,取左、右頸動脈竇下1 cm處分別測量3次,取其均值即為平均CIMT[16]。
1.6 統計學方法
實驗數據采用SPSS17.0軟件進行統計學分析。計量資料以均數±標準差(±s)表示,兩組間均數比較采用檢驗,構成比比較用χ2檢驗,血清FA水平與其他臨床資料間相關性檢驗采用Pearson相關分析,非正態分布資料采用自然對數轉換為正態分布后進行統計學分析。以<0.05為差異有統計學意義。
附表兩組代謝指標與血清FA水平(=100,±s)
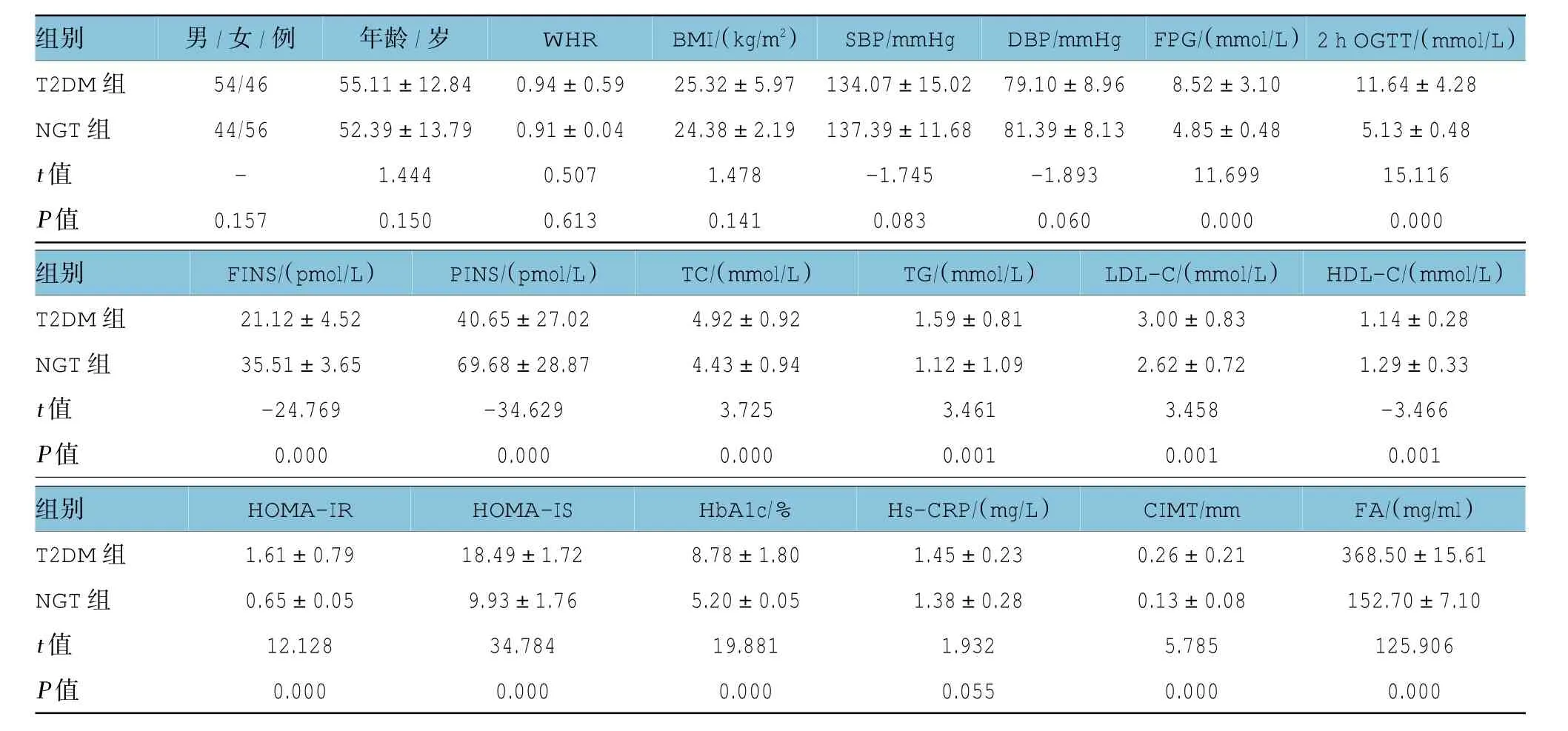
附表兩組代謝指標與血清FA水平(=100,±s)
2 h OGTT/(mmol/L)T2DM組54/4655.11±12.840.94±0.5925.32±5.97134.07±15.0279.10±8.968.52±3.10 11.64±4.28 NGT組44/5652.39±13.790.91±0.0424.38±2.19137.39±11.6881.39±8.134.85±0.485.13±0.48組別男/女/例年齡/歲WHRBMI/(kg/m2)SBP/mmHgDBP/mmHgFPG/(mmol/L)值-1.4440.5071.478-1.745-1.89311.69915.116值0.1570.1500.6130.1410.0830.0600.0000.000組別HDL-C/(mmol/L)T2DM組21.12±4.52 40.65±27.02 4.92±0.92 1.59±0.81 3.00±0.83 1.14±0.28 NGT組35.51±3.6569.68±28.874.43±0.941.12±1.092.62±0.721.29±0.33FINS/(pmol/L)PINS/(pmol/L)TC/(mmol/L)TG/(mmol/L)LDL-C/(mmol/L)值-24.769-34.6293.7253.4613.458-3.466值0.0000.0000.0000.0010.0010.001FA/(mg/ml)T2DM組1.61±0.7918.49±1.728.78±1.801.45±0.230.26±0.21368.50±15.61 NGT組0.65±0.059.93±1.765.20±0.051.38±0.280.13±0.08152.70±7.10組別HOMA-IRHOMA-ISHbA1c/%Hs-CRP/(mg/L)CIMT/mm值12.12834.78419.8811.9325.785125.906值0.0000.0000.0000.0550.0000.000
2 結果
2.1 一般臨床資料比較
兩組臨床資料比較,T2DM組FPG、2h OGTT、FINS、PINS、TC、TG、LDL-C、HDL-C、HOMA-IR、HOMA-IS、HbA1c及CIMT與NGT組比較,差異有統計學意義(<0.05);T2DM組性別分布、年齡、WHR、BMI、SBP、DBP、Hs-CRP與NGT組比較,差異無統計學意義(>0.05)。見附表。
2.2 血清FA水平比較
兩組血清FA水平比較,T2DM組(368.50±15.61)mg/ml>NGT組(152.70±7.10)mg/ml,差異有統計學意義(=125.906,=0.000),見附表。
2.3 FA水平與各項代謝指標的相關性比較
Pearson相關分析結果顯示,FA水平與HOMAIR、CIMT、HbA1c、TG、LDL-C、BMI、SBP、FPG及2 h OGTT呈正相關(=0.483、0.509、0.153、0.353、0.113、0.162、0.182、0.422和0.581,=0.000、0.000、0.042、0.000、0.023、0.024、0.035、0.002和0.000);與FINS、PINS、HDL-C和HOMA-IS呈負相關(=-0.153、-0.423、-0.183、-0.463,=0.008、0.008、0.011和0.000);與TC、DBP和Hs-CRP無相關(>0.05)。見附圖。
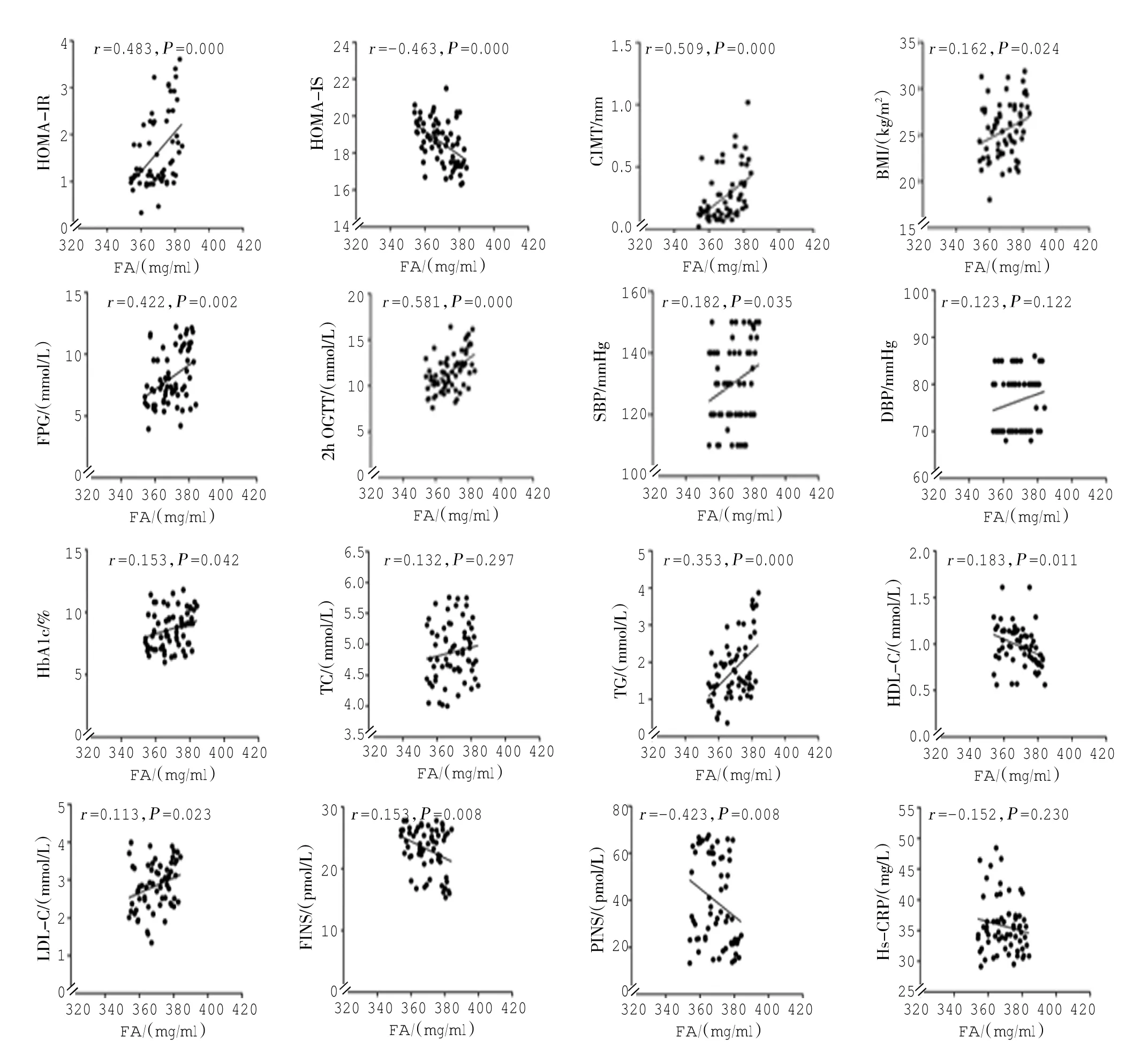
附圖FA水平與各項臨床指標的相關性(Pearson相關分析)
3 討論
FA是由肝臟分泌的一種多功能糖蛋白[17]。有研究表明,FA是DM風險的生物標志物[4-9]。本研究發現,nT2DM患者血清FA水平較NGT組升高。血脂異常是血液中TC、TG、LDL-C水平升高和(或)HDL-C水平降低。HDL-C能夠通過逆向轉運膽固醇、抵抗低密度脂蛋白氧化、保護內皮功能等機制起到抗AS作用,因此在AS中具有保護作用[18]。有研究表明,血清FA水平與內臟型肥胖和血脂異常有關[19-20]。目前研究發現,血清FA水平與LDL-C和TG呈正相關,與HDL-C呈負相關。此外,血清FA水平還與BMI、SBP、HbA1c、FPG和2h OGTT有關。然而,在對照研究中有研究報道[21],FA水平與踝肱指數(ankle brachial index,ABI)呈正相關,而與代謝參數無明顯相關性。
此外,有研究表明,FA水平與IR相關[10,22-23]。本研究結果發現,血清FA水平與HOMA-IR呈正相關,與FINS、PINS和HOMA-IS呈負相關。這些結果表明,FA在nT2DM患者引起IR的過程中可能發揮作用。本研究結果與早期FA和IR相關性研究的數據結果一致。目前研究發現,血清FA水平與CIMT呈正相關,本研究結果表明,血清FA水平可能與nT2DM患者大血管病變有關。
綜上所述,本研究發現nT2DM患者血清FA水平升高,證明nT2DM患者血清FA水平與IR及CIMT之間存在相關性,研究結果表明,血清FA水平可作為診斷nT2DM患者大血管病變的獨立生物學標志物,在DM合并大血管并發癥的發生發展中可能起重要作用。
[1]STAM-SLOB M C,VAN DER GRAAF Y,DE BORST G J,et al.Effect of type 2 diabetes on recurrent major cardiovascular events for patients with symptomatic vascular diseaseat differentlocations[J].Diabetes Care,2015,38(8):1528-1535.
[2]SIBAL L,AGARWAL S C,HOME P D.Carotid intima-media thickness as a surrogate marker of cardiovascular disease in diabetes[J].Diabetes Metabolic Syndrome&Obesity Targets&Therapy,2011,4(4):23-34.
[3]王麗敏,袁慧娟,趙志剛,等.2型糖尿病治療及合并高血壓和高脂血癥情況調查分析[J].中華實用診斷與治療雜志,2015,29(12):1245-1246.
[4]SUN Q,CORNELIS M C,MANSON J E,et al.Plasma levels of fetuin-A and hepatic enzymes and risk of type 2 diabetes in women in the U.S[J].Diabetes,2013,62(1):49-55.
[5]FETHIYE O G,SEMBOL T Y,MUSTAFA T,et al.Serum visfatin and fetuin-A levels and glycemic control in patients with obese type 2 diabetes mellitus[J].Diabetes&Metab Journal,2011,35(5):523-528.
[6]IX J H,BIGGS M L,MUKAMAL K J,et al.Association of fetuin-a with incident diabetes mellitus in community-living older adults:the cardiovascular health study[J].Circulation,2012,125(19):2316-2322.
[7]KANBAY M,NICOLETA M,SELCOKI Y,et al.Fibroblase growth factor 23 and fetuin A are independent predictors for the coronary artery disease extent in mild chronic kidney disease[J].Clin J Am Soc Nephrol,2010,5(10):1780-1786.
[8]LAUGHLIN G A,BARRETT-CONNOR E,CUMMINS K M,et al.The sex-specific association of fetuin-A with type 2 diabetes inoldercommunity-dwellingadults:theRanchoBernardo Study[J].Diabetes Care,2013,36(7):1994-2000.
[9]RASUL S,WAGNER L,KAUTZKY-WILLER A.Fetuin-A and angiopoietins in obesity and type 2 diabetes mellitus[J].Endocrine,2012,42(3):496-505.
[10]SONG A,XU M,BI Y,et al.Serum fetuin-A associates with type 2 diabetes and insulin resistance in Chinese adults[J].PLos One,2011,6(4):e19228.
[11]O’REILLY M,AVALOS G,DENNEDY M C,et al.Breast-feeding is associated with reduced postpartum maternal glucose intolerance after gestational diabetes[J].IrMedJ,2012,105(5 Supp1):31-36.
[12]MATHEWS S T,SINGH G P,RANALLETTA M,et al.Improved insulin sensitivity and resistance to weight gain in mice null for the Ahsg gene[J].Diabetes,2002,51(8):2450-2458.
[13]SCH?FER C,HEISS A,SCHWARZ A,et al.The serum protein alpha 2-Heremans-Schmid glycoprotein/fetuin-A is a systemically acting inhibitor of ectopic calcification[J].Journal of Clinical Investigation,2003,112(3):357-366.
[14]LORANT D P,GRUJICIC M,HOEBAUS C,et al.Fetuin-A levels are increased in patients with type 2 diabetes and peripheral arterial disease[J].Diabetes Care,2011,34(1):156-161.[15]ERASO L H,GINWALA N,QASIM A N,et al.Association of lower plasma fetuin-A levels with peripheral arterial disease in type 2 diabetes[J].Diabetes Care,2010,33(4):408-410.
[16]AYDIN M,BULUR S,ALEMDAR R,et al.The impact of metabolic syndrome on carotid intima media thickness[J].Eur Rev Med Pharmacol Sci,2013,17:2295-2301.
[17]MORI K,EMOTO M,INABA M.Fetuin-A:a multifunctional protein[J].Recent Pat Endocr Metab Immune Drug Discov,2011,5(2):124-126.
[18]LüSCHER T F,LANDMESSER U,VON ECKARDSTEIN A,et al.High-density lipoprotein:vascular protective effects,dysfunction,and potential as therapeutic target[J].Circ Res,2014,114(1):171-182.
[19]XU Y,XU M,BI Y,et al.Serum fetuin-A is correlated with metabolicsyndromeinmiddle-agedandelderlyChinese[J].Atherosclerosis,2011,216(1):180-186.
[20]ISMAIL N A,RAGAB S,DAYEM S A E,et al.Fetuin-A levels in obesity:differences in relation to metabolic syndrome and correlation with clinical and laboratory variables[J].Arch Med Sci,2012,8(5):826-833.
[21]ROOS M,OIKONOMOU D,VON EYNATTEN M,et al.Associations of fetuin-A levels with vascular disease in type 2 diabetes patients with early diabetic nephropathy[J].Cardiovascular Diabetology,2010,9(1):1-7.
[22]OU H Y,YANG Y C,WU H T,et al.Serum fetuin-A concentrations are elevated in subjects with impaired glucose tolerance and newly diagnosed type 2 diabetes[J].Clin Endocrinol(Oxf),2011,75(4):450-455.
[23]ISHIBASHI A,IKEDA Y,OHGURO T,et al.Serum fetuin-A is an independent marker of insulin resistance inJapanese men[J].J Atheroscler Thromb,2010,17(9):925-933.
(張蕾編輯)
Association of fetuin-A level with insulin resistance and carotid intima-media thickness in patients with newly-diagnosed type 2 diabetes mellitus*
Yu-ting Dang,Liang Yin,Kan Sun,Xiang-yun Chang
(Department of Endocrine and Metabolic Diseases,the First Affiliated Hospital,Medical College of Shihezi University,Shihezi,Xinjiang 832002,China)
ObjectiveTo investigate the correlations of fetuin-A(FA)level with insulin resistance(IR)and carotid intima-media thickness(CIMT)in patients with newly-diagnosed type 2 diabetes mellitus(nT2DM).MethodsOne hundred cases of nT2DM patients were selected as experimental group(T2DM group)while 100 people with normal glucose tolerance(NGT)as control group(NGT group).Serum FA level was measured by a commercial solidphase ELISA kit.The estimation of IR was calculated by homeostasis model assessment(HOMA-IR).CIMT was measured by color B-mode ultrasound.The correlations of serum fetuin-A level with the metabolic parameters were also analyzed.ResultsThe serum FA level in the T2DM group was significantly higher than that in the NGT group[(368.5±15.6)vs(152.7±7.1)mg/ml,=0.000].Serum FA level was positively correlated with HOMA-IR(=0.483,=0.000),CIMT(=0.509,=0.000),glycated hemoglobin(=0.153,=0.042),triglyceride(=0.353,=0.000),low-density lipoprotein cholesterol(=0.113,=0.023),body mass index(=0.162,=0.024),systolic blood pressure(=0.182,=0.035),fasting plasma glucose(=0.422,=0.002)and 2-h post-glucose load blood glucose(=0.581,=0.000);but negatively correlated with fasting plasma insulin(=-0.153,=0.008),2-h plasma insulin after glucose load(=-0.423,=0.008),high-density lipoprotein cholesterol(=-0.183,=0.011)and HOMA-β-cell insulin secretion index(=-0.463,=0.000).Conclusions The study demonstrated that serum FA level is correlated with IR and CIMT in patients with nT2DM.Therefore,serum FA level can be used as an independent marker in the diagnosis of macroangiopathies in patients with nT2DM.
newly-diagnosed type 2 diabetes mellitus;fetuin-A;insulin resistance;carotid intima-media thickness
10.3969/j.issn.1005-8982.2017.16.009
1005-8982(2017)16-0044-05
R587.1
A
2016-12-16
國家自然科學基金地區基金項目(No:81560137;No:81560139)
常向云,E-mail:cxyshzdx@126.com

