基于保護動機理論的兒童抽動障礙患者用藥依從性研究
楊春松 張伶俐 李佳圓 俞丹 楊亞亞 吳小芳


編者按:為深入學習貫徹習近平新時代中國特色社會主義思想,落實2021年全國宣傳部長會議和全國衛生健康工作會議精神,聚焦中國共產黨成立以來衛生健康事業歷史進程中的重要決策、活動及成果,從不同角度和層面展現衛生健康事業發展的重要成就,我刊特從2021年7月起開設“黨為人民謀健康的100年”專欄,從我刊實際出發,陸續推出一系列我國健康衛生事業與藥學工作結合的相關文章,從而助力提高人民健康水平制度保障、堅持和發展中國特色衛生健康制度。本期專欄文章《基于保護動機理論的兒童抽動障礙患者用藥依從性研究》以317例兒童抽動障礙患者為研究對象,以強調行為主體對行為長期認知的調節作用的“保護動機理論”作為理論基礎,采用調查問卷收集患者用藥依從性和相關因素數據,并采用結構方程模型分析對用藥依從性有顯著影響的重要因素,進而針對性地提出兒童抽動障礙患者用藥管理策略,從而為改善藥物治療效果、提升醫療機構兒科醫務工作者的服務水平提供參考。
中圖分類號 R725.9;R971;R985 文獻標志碼 A 文章編號 1001-0408(2021)19-2415-06
DOI 10.6039/j.issn.1001-0408.2021.19.19
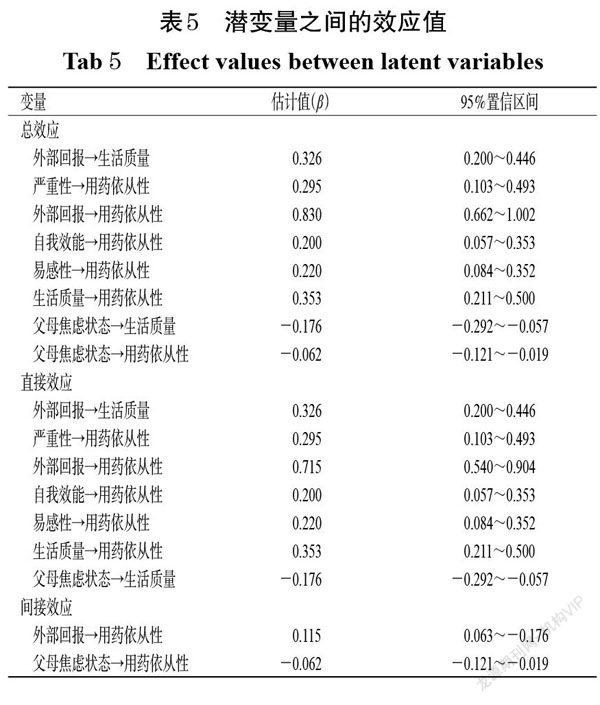
摘 要 目的:研究兒童抽動障礙(TD)患者用藥依從性現狀及影響因素,為改善兒童TD患者的用藥依從性提供依據。方法:基于保護動機理論設計調查問卷,采用橫斷面調查研究方法于2018年1月-2019年12月對四川大學華西第二醫院確診的兒童TD患者進行問卷調查,并根據理論假設建立結構方程模型,采用極大似然法估計模型;對單因素分析中有顯著影響的因素進行多元線性回歸分析,并開展路徑分析和中介效應檢驗。結果:共納入317例患者,平均年齡為(8.38±2.54)歲,平均病程為(3.19±2.46)年;用藥依從性平均得分為(5.70±1.69)分,其中15.1%為依從性低,37.5%為依從性中等,47.3%為依從性高。多元線性回歸分析顯示,有無共患病(β=0.124,SE=0.167,P=0.011)、主要監護人受教育程度(β=0.236,SE=0.110,P<0.000 1)、生活質量(β=0.399,SE=0.112,P<0.000 1)和服用藥物種類(β=0.166,SE=0.047,P=0.001)是影響兒童TD患者用藥依從性的影響因素。結構方程模型分析顯示,嚴重性(β=0.295,95%置信區間:0.103~0.493)、外部回報(β=0.830,95%置信區間:0.662~1.002)、自我效能(β=0.200,95%置信區間:0.057~0.353)、易感性(β=0.220,95%置信區間:0.084~0.352)和生活質量(β=0.353,95%置信區間:0.211~0.500)對患者用藥依從性均有直接的正向影響,生活質量在外部回報和依從性變量之間起中介作用(中介效應占總效應值的13.9%)。結論:兒童TD患者用藥依從性不高;建議各級醫療機構的兒科醫務工作者從嚴重性、易感性、外部回報和自我效能去管理患者的用藥依從性,以提高患者及其監護人對疾病及用藥不依從的嚴重性和易感性的認識,同時弱化外部回報和增加自我效能,最終提升患者的用藥依從性。
關鍵詞 兒童;抽動障礙;用藥依從性;保護動機理論;結構方程模型;影響因素
Study on the Medication Compliance of Children with Tic Disorder Based on the Theory of Protective Motivation
YANG Chunsong1,2,ZHANG Lingli1,2,LI Jiayuan3,YU Dan4,YANG Yaya1,2,WU Xiaofang1(1. Dept. of Pharmacy, West China Second Hospital of Sichuan University/Evidence-based Pharmacy Center, Chengdu 610041, China; 2. Key Laboratory of Obstetric & Gynecologic and Pediatric Diseases and Birth Defects of Ministry of Education, Sichuan University, Chengdu 610041, China; 3. West China School of Public Health, Sichuan University/Discipline Construction Department of West China Fourth Hospital, Chengdu 610041, China; 4. Dept. of Genetics, Metabolism and Endocrinology, West China Second Hospital of Sichuan University, Chengdu 610041, China)
ABSTRACT ? OBJECTIVE: To study the current status and influencing factors of medication compliance in children with tic disorder (TD), and to provide reference for improving medication compliance in TD children. METHODS: The questionnaire was designed according to the protection motivation theory. The cross-sectional study was adopted to conduct questionnaire survey among TD children in West China Second Hospital of Sichuan University from Jan. 2018 to Dec. 2019. The structural equation model was established according to the theoretical assumptions, and the maximum likelihood method was used to estimate the model; multiple linear regression analysis was carried out for the factors with significant influence in the single factor analysis, and path analysis and intermediary effect test were carried out. RESULTS: A total of 317 patients with TD were included, the mean age was (8.38±2.54) years, and the mean course of disease was (3.19±2.46) years. Average medication compliance scores was (5.70±1.69), among which 15.1% was low compliance, 37.5% moderate compliance, and 47.3% high compliance. Multivariate linear regression analysis showed that comorbidities (β=0.124, SE=0.167, P=0.011), education level of the main guardian (β=0.236, SE=0.110, P<0.001), quality of life (β=0.399, SE=0.112, P<0.001) and the types of drugs taken (β=0.166, SE=0.047, P=0.001) were the factors affecting medication compliance of children with TD. Structural equation model analysis showed that severity (β=0.295,95%CI:0.103-0.493), external return (β=0.830,95%CI:0.662-1.002), self-efficacy (β=0.200,95%CI:0.057-0.353), susceptibility (β=0.220,95%CI:0.084-0.352) and quality of life (β=0.353,95%CI:0.211-0.500) had a direct positive impact on medication compliance. Quality of life mediated between external returns and compliance variables (intermediary effect accounted for 13.9% of the total effect value). CONCLUSIONS: Children with TD have low medication compliance. It is recommended that pediatricians in medical institutions at all levels to manage the medication compliance of patients with TD from the severity, susceptibility, external returns and self-efficacy, so as to improve patients and guardians awareness of the severity and susceptibility of disease and medication non-adherence, weaken external returns and increase self-efficacy, and ultimately improve medication compliance of patients.

