單孔胸腔鏡手術在結核性膿胸治療中的應用
鄧高焱 王永利 范明 何超 王勛 吳郁美 石自力
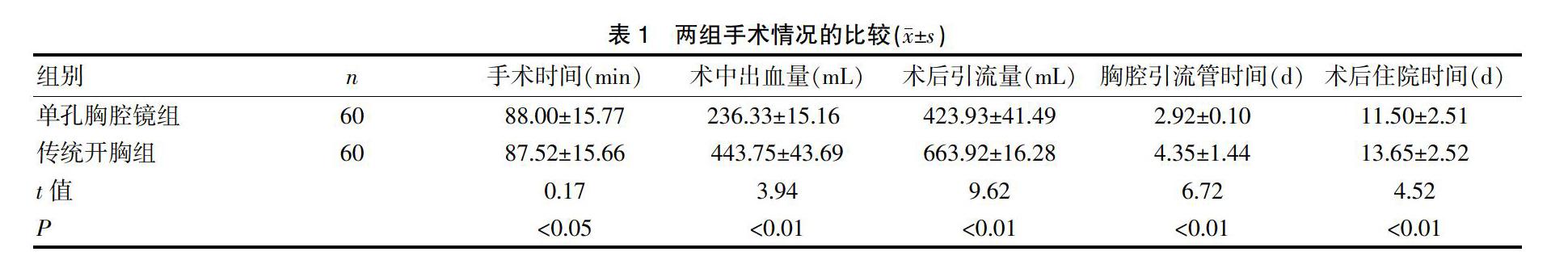
[摘要] 目的 探討單孔胸腔鏡手術治療結核性膿胸的應用價值,并總結相關臨床經驗。 方法 回顧性分析我院胸外科2015年1月~2017年12月住院手術治療的120例結核性膿胸患者。依據納入、排除的相關標準,在知情同意下將納入患者隨機分為研究組(單孔胸腔鏡手術組,60例)和對照組(傳統開胸手術組,60例),比較兩組患者的手術時間、術中出血量、術后引流量、胸腔引流管時間、術后住院時間及術后并發癥。 結果 兩組患者圍術期均無死亡病例,中轉開胸3例,中轉開胸率為5%(3/60)。單孔胸腔鏡組與傳統開胸組相比較,手術時間分別為(88.00±15.77)min、(87.52±15.66)min,術中出血量分別為(236.33±15.16)mL、(443.75±43.69)mL,術后引流量分別為(423.93±41.49)mL、(663.92±16.28)mL,胸腔引流管時間分別為(2.92±0.10)d、(4.35±1.44)d,術后住院時間分別為(11.50±2.51)d、(13.65±2.52)d,兩組患者的術中出血量、術后引流量、胸腔引流管時間及術后住院時間相比,差異均有統計學意義(P均<0.05)。比較兩組的手術時間,差異無統計學意義(P>0.05)。單孔胸腔鏡組術后并發癥的總的發生率為6.67%(4/60),傳統開胸組術后并發癥的總發生率為13.33%(8/60)。 結論 單孔胸腔鏡手術治療結核性膿胸創傷小、并發癥少、住院時間短,患者恢復快,在臨床應用中值得推廣。但在臨床實際中應根據患者病情合理選擇手術方式。
[關鍵詞] 單孔胸腔鏡;膿胸;結核性;手術
[中圖分類號] R521.7? ? ? ? ? [文獻標識碼] B? ? ? ? ? [文章編號] 1673-9701(2020)04-0050-04
Application of single-port thoracoscopic surgery in the treatment of tuberculous empyema
DENG Gaoyan? ?WANG Yongli? ?FAN Ming? ?HE Chao? ?WANG Xun? ?WU Yumei? ?SHI Zili
Department of Thoracic Surgery, Hunan Chest Hospital, Changsha? ?410013, China
[Abstract] Objective To investigate the application value of single-port thoracoscopic surgery for tuberculous empyema and to summarize relevant clinical experience. Methods 120 patients with tuberculous empyema who underwent surgical treatment from January 2015 to December 2017 in the Department of Thoracic Surgery of Hospital were retrospectively analyzed. According to the relevant criteria of inclusion and exclusion, the patients were randomLy divided into the study group (single-port thoracoscopic surgery group, 60 cases) and the control group (traditional thoracotomy group, 60 cases) with informed consent. Surgical time, intraoperative blood loss, postoperative drainage, chest drainage time, postoperative hospital stay, and postoperative complications between two groups were compared. Results There were no deaths in the perioperative period, and 3 cases were converted to thoracotomy. The conversion rate of thoracotomy was 5%(3/60). In the single-port thoracoscopic surgery group and the traditional thoracotomy group, the operation time was (88.00±15.77) min and (87.52±15.66) min, respectively; the intraoperative blood loss was (236.33±15.16) mL and (443.75±43.69) mL, respectively; the post-drainage was (423.93±41.49) mL and (663.92±16.28) mL, respectively; the chest drainage time was(2.92±0.10)d,(4.35±1.44) d, respectively; the postoperative hospital stay was (11.50±2.51)d, (13.65±2.52)d. There were significant differences in the intraoperative blood loss, postoperative drainage, chest drainage time and postoperative hospital stay(P<0.05). There was no significant difference in the operation time between the two groups(P>0.05). The overall incidence of postoperative complications in the single-port thoracoscopic surgery group was 6.67%(4/60), and the overall incidence of postoperative complications in the traditional thoracotomy group was 13.33%(8/60). Conclusion Single-port thoracoscopic surgery in the treatment of tuberculous empyema has less trauma, fewer complications, shorter hospital stay, and faster recovery. It is worthy of promotion in clinical application. However, in clinical practice, the surgical method should be reasonably selected according to the patient's condition.
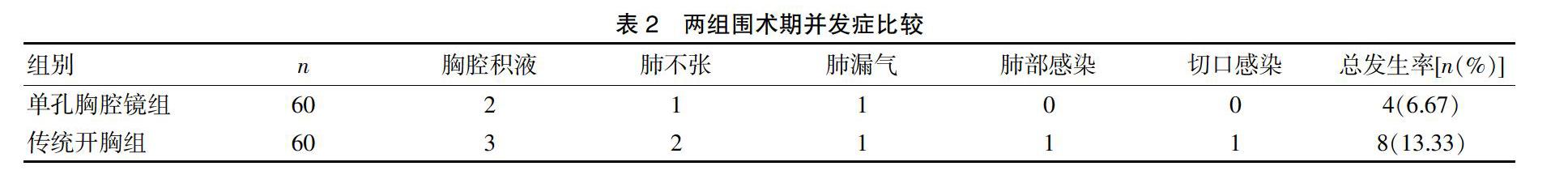
2.2 兩組圍術期并發癥比較
圍術期并發癥主要包括胸腔積液、肺不張、肺漏氣、肺部感染、切口感染,單孔胸腔鏡組圍術期出現胸腔積液2例,肺不張1例,肺漏氣1例,無肺部感染及切口感染病例,總的并發癥發生率為6.67%(4/60)。傳統開胸組圍術期出現胸腔積液3例,肺不張2例,肺漏氣1例,肺部感染1例,切口感染1例,總的并發癥發生率為13.33%(8/60)。見表2。
3 討論
結核病嚴重影響人類的健康,目前我國的結核疫情形式嚴峻,世界衛生組織(World Health Organization,WHO)把印度、中國、俄羅斯、南非等22個國家列為結核病高負擔、高危險性國家,中國居世界第二位[4]。目前結核治療方案包括藥物、手術、免疫、營養等多種手段的綜合治療[5]。對結核病及時、正確的診斷、治療,不僅有利于患者康復,而且對消除傳染源、控制結核疫情至關重要。
空洞型肺結核,早期胸膜炎未及時或規范治療,耐藥結核菌,胸壁、脊柱旁結核膿腫破潰或直接蔓延等多種因素是結核性膿胸形成原因,結核性膿胸的病理過程包括滲出期、纖維素期及機化期[6]。美國胸科協會(AST)將結核性膿胸分為滲出期膿胸(Ⅰ期),纖維素期膿胸(Ⅱ期),機化期膿胸(Ⅲ期)[7]。早期結核性膿胸未經規范化治療可出現胸廓塌陷、支氣管胸膜瘺、胸壁破潰流膿、心肺功能受損等并發癥。積極的外科手術干預對Ⅰ、Ⅱ期結核性膿胸患者康復具有良好的臨床效果,國內外對結核性膿胸的手術適應證及術式仍未形成統一的共識,目前手術方式主要包括傳統開胸手術、電視胸腔鏡手術及胸腔鏡輔助小切口手術[8]。胸腔鏡手術相比于傳統開胸手術的主要優勢為創傷小、出血量少、術后疼痛較輕、并發癥少,主要劣勢為操作空間小、病灶難以徹底清除[7]。本研究對比分析兩組手術患者的術中出血量、術后引流量、胸腔引流管時間及術后住院時間,單孔胸腔鏡手術較傳統開胸手術具有明顯的優勢,與相關文獻的觀點接近[9]。比較分析兩組患者的手術時間,兩組患者無明顯差異,本研究認為單孔胸腔鏡暴露視野不如傳統開胸手術,操作空間小,操作難度較大,同時也與手術醫師的操作技能有關。
本研究中有3例患者術中中轉開胸,其中2例為術中大出血,1例胸腔臟壁粘連嚴重。1例術中出現大出血的患者為Ⅲ期膿胸患者,胸膜纖維板增厚及部分胸膜鈣化,分界不清,不易剝離。機化期膿胸(Ⅲ期)常出現胸廓塌陷,肋間隙狹窄,脊柱側彎,手術操作難度大,術中容易損傷肺組織導致大出血,增厚胸膜分界不清使膈肌破裂,誤傷腹腔臟器,術后出現支氣管胸膜瘺或肺瘺的風險增加[10-11]。1例為術中損傷肺靜脈,出血量大,從手術安全角度考慮中轉開胸。1例為全胸腔粘連,病程超過3個月,操作難度大。筆者認為單孔胸腔鏡治療結核性膿性最好選取Ⅰ、Ⅱ期患者,胸腔鏡下易完整剝離纖維板,術中肺組織牽拉少,出血量少,肺復張好。部分Ⅲ期初期如胸腔粘連輕亦可嘗試選擇,操作者需具備嫻熟的胸腔鏡操作技能,盲目的追求微創手術容易導致胸膜纖維板剝離不徹底、創面滲血增多、肺組織破損多及術后瘺氣時間長等并發癥的增加,此類患者胸腔鏡輔助小切口手術可作為備選項[8]。結核性膿胸胸腔粘連較重,掌握好粘連分離的原則可減少手術時間、減少出血量、降低操作難度。本研究認為一般而言應先分離粘連較輕處,再分離粘連較重處,或先分離視野暴露好、易分離處,先易后難。
與傳統開胸手術相比,胸腔鏡手術并發癥少[12]。Marks DJB等[13]研究認為胸腔鏡膿胸剝脫術在肺功能保護、快速康復、減少疼痛等方面較傳統開胸手術具有明顯優勢。本研究中主要并發癥包括胸腔積液、肺不張、肺漏氣、肺部感染、切口感染,胸腔積液的原因包括胸腔引流管位置較高、術后傷口疼痛、術后營養差等,單孔胸腔鏡組有2例出現胸腔積液,傳統開胸組有3例,本研究認為單孔胸腔鏡組術后引流管在操作孔下緣,相比于傳統開胸組引流管位置較高,引流效果較差。傳統開胸組術后出現肺不張、肺部感染的概率較單孔胸腔鏡組高,主要考慮為手術創面大,疼痛難忍,患者術后咳嗽、吹氣球等依從性差。如患者術后傷口疼痛難忍可使用止痛藥,鼓勵患者咳嗽、咳痰。對于術后傷口疼痛難忍患者待胸腔引流液減少后可盡早拔除胸腔引流管,減輕患者疼痛,在CT或彩超引導下置入胸腔微管(一般使用中心靜脈導管),或術中常規留置胸腔微管,術后間斷予以尿激酶胸腔沖管,引流效果佳。本研究中出現術后持續漏氣2例,均為胸腔粘連重,術中剝離面大,出現較大的肺破口,均采用持續留置胸腔引流管,囑患者加強營養,保守治療后痊愈,此外部分文獻報道對于持續性漏氣可以使用高滲葡萄糖和(或)自體血胸腔注射效果良好[14-15]。結核性膿胸為Ⅲ類切口,術后出現切口感染的概率較Ⅰ、Ⅱ類切口高,術前規律抗結核6~8周可降低術后切口感染發生率。本研究中傳統開胸組出現切口感染1例,患者合并2型糖尿病,術前血糖控制欠佳,主要與手術創面大及術后血糖控制欠佳有關。圍術期血糖控制在6.0~10.0 mmol/L能有效的減少切口感染發生率[16]。
總之,與傳統的開胸手術相比,單孔胸腔鏡手術治療Ⅰ、Ⅱ期結核性膿胸創傷小、并發癥少、住院時間短,在臨床應用中值得推廣,但對于Ⅲ期的結核性膿胸患者應慎重,在臨床實際中的應根據具體情況合理選擇手術方式。
[參考文獻]
[1] 張運曾,金鋒,王成.電視輔助胸腔鏡手術在結核性膿胸治療中的應用及進展[J].中國防癆雜志,2017,39(5):525-528.
[2] 李向紅,李萬志.結核性膿胸126例臨床分析[J].中國現代醫生,2010,48(8):118-119.
[3] Kumar A,Asaf BB,Lingaraju VC,et al. Thoracoscopic decortication of stage Ⅲ tuberculous empyema is effective and safe in selected cases.[J]. Annals of Thoracic Surgery,2017,104(5):S0003497517309207.
[4] Biritwum RB,Minicuci N,Yawson AE,et al. Prevalence of and factors associated with frailty and disability in older adults from China,Ghana,India,Mexico,Russia and South Africa[J]. Maturitas,2016,91:8-18.
[5] 崖宇翔.伴合并癥的肺結核治療研究進展[J].心理醫生,2016,22(34):3-4.
[6] Terzi A,Bertolaccini L,Gorla A,et al. Surgery for the treatment of the tuberculosis-destroyed lung:To protect or not to protect the bronchial stump?[J]. European Journal of Cardio-Thoracic Surgery:Official Journal of the European Association for Cardio-thoracic Surgery,2013, 43(1):201.
[7] Lee SF,Lawrence D,Booth H,et al. Thoracic empyema:Current opinions in medical and surgical management[J].Current Opinion in Pulmonary Medicine,2010,16(3):194.
[8] Barbetakis N,Paliouras D,Asteriou C,et al. Comment:The role of video-assisted thoracoscopic surgery in the management of tuberculousempyemas[J]. Interactive Cardiovascular & Thoracic Surgery,2009,8(3):337.
[9] 徐寧,湯磊,朱峰,等.電視胸腔鏡手術治療結核性膿胸的臨床療效分析[J].中國防癆雜志,2017,39(5):459-463.
[10] Kundu S,Mitra S,Mukherjee S,et al. Adult thoracic empyema:A comparative analysis of tuberculous and nontuberculous etiology in 75 patients[J]. Lung India Official Organ of Indian Chest Society,2010,27(4):196-201.
[11] 鄧勇軍,劉煥鵬,喻應洪,等.改良胸腔鏡下胸膜纖維板剝脫術治療慢性膿胸31例[J].中國微創外科雜志,2016, 16(11):1009-1012.
[12] Zhao L,Cao S,Zhu C,et al. Application of thoracoscopic hybrid surgery in the treatment of stage III tuberculous empyema[J].Ann Thorac Cardiovasc Surg,2015,21(6):523-528.
[13] Marks DJB,Fisk MD,Koo CY,et al. Thoracic Empyema:A 12-Year study from a UK Tertiary Cardiothoracic Referral Centre[J]. Plos One,2012,7(1):e30074.
[14] Oliveira FHS,Cataneo DC,Ruiz RL,et al. Persistent pleuropulmonary air leak treated with autologous blood:Results from a university hospital and review of literature[J].Respiration,2010,79(4):302-306.
[15] Fujino K,Motooka Y,Koga T,et al. Novel approach to pleurodesis with 50% glucose for air leakage after lung resection or pneumothorax[J].Surgery Today,2016,46(5):599-602.
[16] 彭海軍,段小亮,李建行,等.肺結核合并2型糖尿病患者行電視胸腔鏡手術治療的臨床分析[J].醫學理論與實踐,2014,(16):2109-2111.
(收稿日期:2019-10-12)

